Implants
Dental Implants
People are living longer than ever, and while regular brushing, flossing, and checkups allow many of us to maintain our natural smiles for a lifetime, sometimes our teeth just can't keep up. If you've lost a tooth (or a few teeth) due to injury or disease, dental implants can rejuvenate both your smile and your oral health.
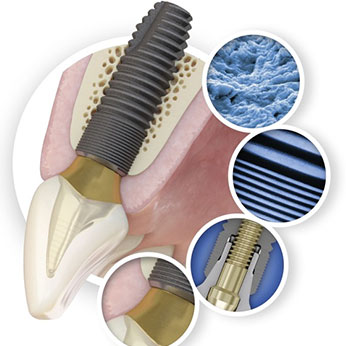
An implant is a synthetic tooth root in the shape of a post that is surgically placed into the jawbone. The “root” is usually made of titanium (the same material used in many replacement hips and knees), a metal that is well suited to pairing with human bone. A replacement tooth is then fixed to the implant. The tooth can be either permanently attached or removable.
The ideal candidate for implants is a non-smoker who has good oral health, including a sufficient amount of bone in the jaw and healthy gums with no sign of gum disease.
Single or Multiple Implants
Implants are versatile. If you are missing only one tooth, one implant plus one replacement tooth will do the trick. If you are missing several teeth in a row, a few strategically placed implants can support a permanent bridge (a set of replacement teeth). Similarly, if you have lost all of your teeth, a full bridge or full denture can be permanently fixed in your mouth with a strategic number of implants.
Advantages Over Dentures or Bridges
Conventional full and partial dentures are not fixed to the bone, and can, therefore, be unstable. This can make it difficult to eat or smile with confidence. Implants not only look more natural but feel and act more like normal teeth, with a stronger biting force. And because they don't directly rely on neighboring teeth for support, implants don't compromise the health of your natural teeth. Fixed bridges that are permanently attached to neighboring teeth are only expected to last seven to ten years whereas implants may outlive you.
Post-Treatment Care
Consider your replacement teeth to be the same as natural teeth. They require the same daily brushing and flossing, and the same number of regular checkups. Just like your natural teeth, the better you take care of your replacements the longer they will last.